
Highlights of the 2020 AHA Guidelines Update for CPR
Every few years, the American Heart Association updates its guidelines for advanced cardiac life support (ACLS). These updates take into account all the new research and medical discoveries that have occurred recently. The goal is to ensure patients receive the best possible care. The recent 2020 update resulted in some changes to AHA CPR guidelines. Being aware of these changes can potentially have life-saving results, so here are the main highlights you need to be aware of before performing CPR.
New Focus on Expanding CPR Training in the AHA 2020 Guidelines
A particularly interesting facet of the 2020 AHA update is the recommendation for who should have CPR training in the first place. Many people are under the impression that only professionals should conduct CPR and that they should only do so if a patient doesn’t have a pulse. However, the new guidelines emphasize that the potential benefits of CPR far outweigh the risks when the patient is unconscious or struggling to breathe.
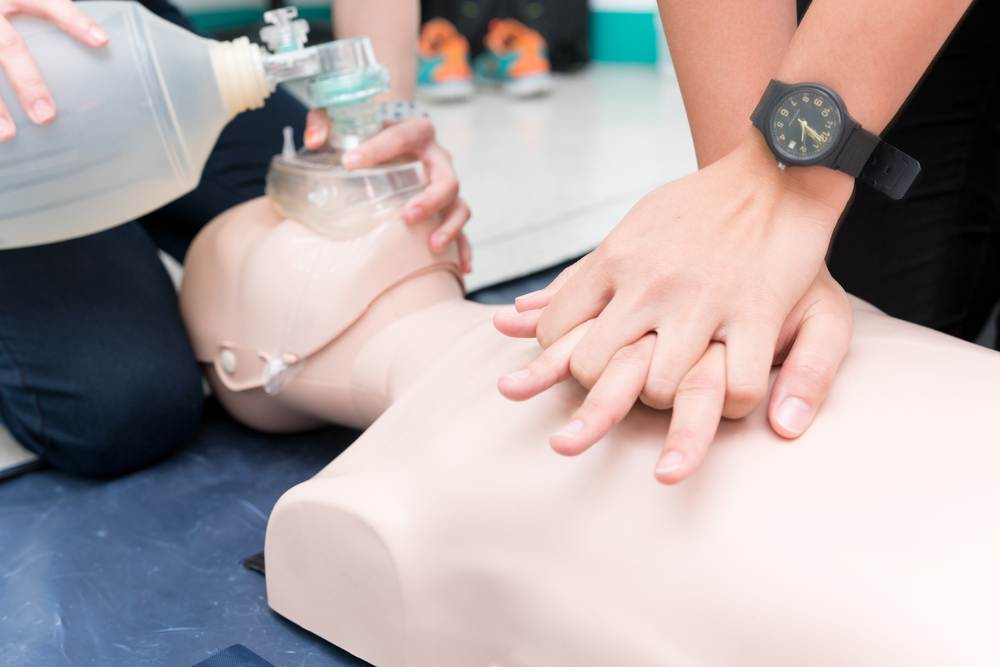 Their findings have discovered there’s a low risk of harm if a person who isn’t in cardiac arrest receives CPR. Therefore, they now recommend a “better safe than sorry” approach. If a bystander notices someone exhibiting the signs of cardiac arrest, such as struggling to breathe, they should attempt to administer CPR—especially if they can’t find a pulse.
Their findings have discovered there’s a low risk of harm if a person who isn’t in cardiac arrest receives CPR. Therefore, they now recommend a “better safe than sorry” approach. If a bystander notices someone exhibiting the signs of cardiac arrest, such as struggling to breathe, they should attempt to administer CPR—especially if they can’t find a pulse.
Since the new guidelines suggest bystanders perform CPR anytime a patient seems to be in cardiac arrest, there’s a great benefit to having a wide range of people trained in CPR. However, the 2020 AHA CPR guidelines recognize that women, minorities, and those at a lower socioeconomic level are less likely to receive CPR training and perform CPR. The AHA, therefore, recommends enhancing CPR training across a variety of demographics. Suggested ways of improving bystander willingness to perform CPR include:
- Promoting Hands-Only CPR as an alternative to hand and mouth CPR
- Using training methods like virtual reality that turn CPR training into a game
- Tailoring CPR training based on individual cultural and ethnic concerns
- Improving awareness on how to perform CPR on women without inappropriate touching
- Creating videos to help with self-directed CPR training
Updated AHA CPR Guidelines Suggest Involving More Technology
Bystanders can perform CPR with nothing more than their own two hands. However, the new update acknowledges that involving technology greatly improves the chances of CPR success. New research indicates that continually measuring arterial blood pressure and end-tidal carbon dioxide levels during CPR may help the responder to optimize their performance. Therefore, first responders who have access to this sort of monitoring equipment should use it during CPR. If an endotracheal tube and arterial line are present, targeting CPR compressions to an end-tidal carbon dioxide value of at least 10mmHg can be very useful as a guide for improved CPR quality.
Another type of equipment that may prove helpful during CPR is audiovisual feedback. An increasing number of defibrillators in public spaces have technology that gives real-time feedback on CPR performance. They can even help a layperson with minimal training to perform CPR effectively. The AHA 2020 guidelines note that there’s been a 25% increase in survival rates among cases where feedback could help a CPR performer adjust their compression depth and recoil. Another suggested method of providing feedback is training emergency dispatchers to give feedback over the phone.

2020 AHA CPR Guidelines Include Opioid-Specific Recommendations
The nation is currently in the middle of an opioid use crisis, so AHA hypertension guidelines 2020 and CPR guidelines reflect a growing interest in preventing fatal opioid overdoses. When patients overdose on opioids, they often go into cardiac arrest and can benefit from CPR. However, cardiac arrest may present slightly differently when a person has recently taken opioids. Being aware of the differences can save lives.
Therefore, the AHA has created guidelines that will let first responders determine if a person needs CPR following an overdose. Their first recommendation is that CPR may be helpful whenever a person suspected of opioid overdose isn’t breathing normally. This includes any slowed breathing, rapid breathing, or uneven breathing. It’s not recommended that the average bystander check for a pulse since it’s extremely easy to miss a pulse in a person overdosing on opioids. However, if the person is breathing abnormally and a first responder cannot find a pulse, the AHA recommendations also include using an AED and naloxone alongside the CPR.
Early Epinephrine Administration Is Now Approved in AHA CPR Guidelines
The AHA explains that new studies have found that epinephrine is more effective when administered early on. Previous guidelines tended to recommend trying CPR for quite a while before resorting to an epinephrine dosage. However, newer research indicates it’s a good idea to go ahead and administer epinephrine within five minutes of starting chest compressions. This update to the guideline is especially important for pediatric patients. Those who got epinephrine within the first five minutes of CPR were five times as likely to survive to a hospital discharge.
More Rapid Rescue Breath Rates Work Well for Children
Many of the AHA updates focus on pediatric care because there’s been a lot more data on how to help young patients and infants survive cardiac arrest. One of their most major changes is in the timing they recommend for performing CPR. In situations where the person performing CPR is also providing rescue breaths, the AHA recommends giving a rescue breath every two to three seconds. This is a big change from the previous guidelines that suggested a rescue breath every five to six seconds. The change helps accommodate the different oxygen needs of younger patients.
AHA 2020 Guidelines Emphasize the Importance of Continued Care
A final important update is the focus on post-CPR care. A lot of people are under the impression that you can just perform CPR until the patient starts breathing on their own and then step back. However, research shows that ongoing support is useful when patients are recovering from cardiac arrest.
Even after discharge from the hospital, some CPR patients may still suffer from various healthcare problems. Therefore, the AHA recommends hospitals take the time to assess cardiac arrest survivors for any physical, neurological, or cognitive impairments following their cardiac arrests. Doing so before discharging patients can ensure they’re properly supported during their recovery.
So are you interested in getting up to date on all the new guidelines? AZ ACLS is here to help. Our mobile CPR, ACLS, and PALS classes give you the tools you need to help others stay safe. If you’re interested in getting certified under the new AHA updates, click or call now to schedule an appointment.

No Comments
Sorry, the comment form is closed at this time.